At the Bedside: Baby born with organs outside his body healed through care and surgery with UTHealth Houston team

KuoJen Tsao, MD, oversaw the treatment and performed the surgery for Tristan Oliver's large omphalocole, where the organs develop outside the abdomen. (Photo by UTHealth Houston)
Defense attorneys Rick Oliver and Kate Ferrell were thrilled when they saw the printout of their unborn son’s 12-week sonogram.
“We were oohing and aahing,” Ferrell said. “I remember this so clearly.”
But the joy soon turned to alarm when the technician said they needed to talk to a specialist.
“The baby looked like he was holding a pillow, and I’m not a medical professional, so I didn’t realize he was holding a ‘something,’” Oliver said.
What Oliver thought looked like a pillow was actually the baby’s liver, stomach, and intestines, which were growing outside of his abdomen in a sac protected by a thin membrane.
“The tech said they wanted the doctor to come talk to us about an omphalocele and chances of survival, and I am not sure I heard a single word after that,” Oliver said.
Told not to do a search on the term, it was the first thing they did when they got to the car. They drove around, Ferrell said, trying to process the information.
“I freaked out,” she said. “The omphalocele spectrum is insane and no two are the same. It was the scariest thing I ever Googled.”
An omphalocele is a birth defect of the abdominal wall, which allows the infant’s intestines, liver, or other organs to grow outside the belly through the opening of the umbilical cord. As a result, the abdominal cavity may not grow to its normal size and the lungs may be affected. An estimated 1 in 4,200 babies in the U.S. are born with an omphalocele. In some cases, the babies may have other birth defects and chromosomal abnormalities.
If the omphalocele is small, a surgery might be able to be performed right after birth to close the defect. But in cases where the omphalocele is large, repair is usually done when the child is older and in stages.
Ferrell, who was documenting their journey on Facebook, reached out to friends and asked for recommendations for a surgeon. A friend who is a nurse anesthetist recommended KuoJen Tsao, MD, professor and chief of the Division of General and Thoracic Pediatric Surgery, co-director of UTHealth Houston Fetal Center, and The Children’s Fund, Inc. Distinguished Professor in Pediatric Surgery with McGovern Medical School.
After looking at the sonogram images, Tsao recommended waiting until Tristan was older because the omphalocele was fairly large.
“It’s usually better to wait if we have any concerns because we don’t want to cause any harm by prematurely trying to force the organs inside,” Tsao said.
“My first take on Dr. Tsao was that he was competent and confident and could do what I could not do, which was give Katie some peace of mind,” Oliver said. “He drew a picture and I watched her response. It put me at ease because it put her at ease.”
The delivery via C-section occurred when Ferrell was 37 weeks pregnant.
“Rick said there were tons of people in the room and Dr. Tsao and respiratory were on standby,” Ferrell said.
While sonograms appeared to show that Tristan’s lungs were growing properly, his parents were relieved to hear him cry.

Tristan Oliver was born with an omphalocele, where the organs form outside the body. (Photo courtesy of Kate Ferrell)
“The best sound I ever heard is when he came out crying because that meant his lungs were strong. He came out screaming. It makes me cry to this day,” Ferrell said.
She was in the recovery room when she received a surprise visitor: “The next thing I knew, Dr. Tsao wheeled Tristan in, so I could hold his hand. He said, ‘He was doing so well, let’s go let mom see.’ So, I got to see him right away.”
Oliver snapped a photo of the two of them. Then he took a look at the omphalocele.
“It was like the world’s scariest snow globe,” Oliver said. “He was exposed for like 10 seconds and then they put a piece of plastic over it and I was like, ‘Nobody move, don’t touch it, don’t breathe.’ It was a breath-trapped-in-the-throat moment.”
Tsao recommended that they do what’s called “paint and wait,” where the sac is “painted” with an antiseptic and an antibiotic cream. Over time, the baby’s skin will grow over it.
“The antibiotic salve that we put on the membrane is to keep it moist,” said Tsao, who sees patients at UT Physicians. “You don’t want it to dry and crack and break open. We let it scab over and it’s like a magic shell. A crust forms on top and the skin from the edges grows over it, like a wound that needs to be healed. We wait until there is a low risk of the wound opening up before we send them home.”
Parents are trained on how to cover the omphalocele and wrap the abdomen with a bandage to slowly move the organs into place. Anticipated to be in the neonatal intensive care unit for five or six months, Tristan was able to go home just 34 days later.
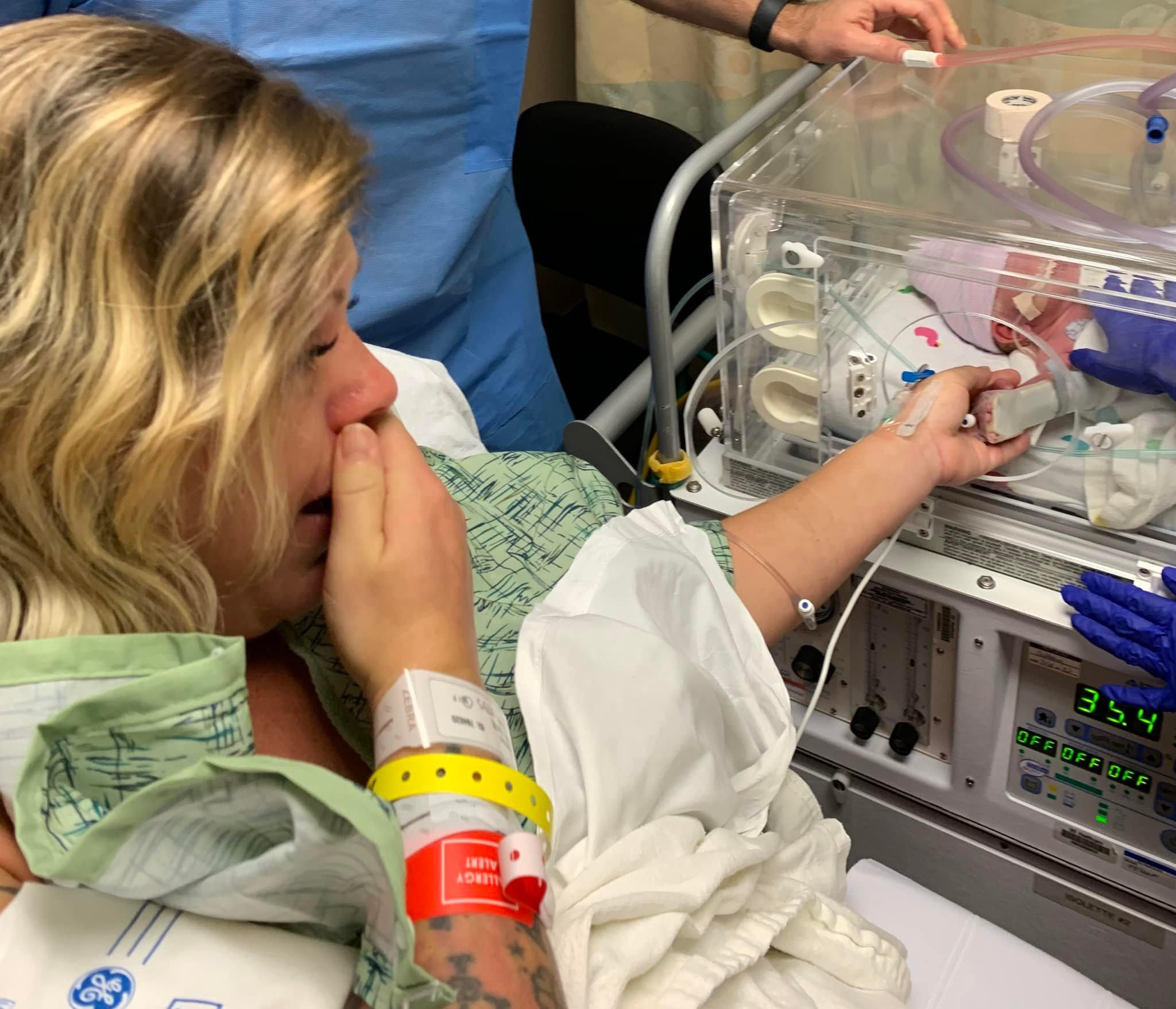
KuoJen Tsao, MD, made sure mom Kate Ferrell could see Tristan right after birth. (Photo by Rick Oliver)
“Part of the success of Tristan’s procedure is the dedication and commitment on the part of the parents,” Tsao said. “All the therapy after they leave the hospital is done by the family: they keep it clean, put salve on it, and wrap it every day. Their care made it easier to do the surgery.”
Oliver said he began to feel better about Tristan’s fragility as the sac was covered with skin.
“I was always amazed by how Dr. Tsao could handle it and not look like he was handling a nuclear device. That something so consequential could be a manageable scab in a matter of months was miraculous,” Oliver said.
The surgery, which brought the muscles and fascia together to seal the abdominal wall, took place at Children’s Memorial Hermann Hospital when Tristan was 15 months old in December 2020.
Once again, he beat expectations. “We were told he would be in the hospital for three to four weeks after surgery, but he went home in three days,” Ferrell said. “This kid is just incredible.”
Tristan, now 4, is lively, according to his parents.
“He is the most rough-and-tumble kid. If he’s not in the mud, he’s trying to climb a tree, or ride his bike. Dr. Tsao said to just let him be a kid, so I just let him be a kid,” Ferrell said. “It was such an all-consuming thing, and looking back, I forget that sometimes. Dr. Tsao — I owe that man everything.”



